The supportive care needs for prostate cancer patients in Sarawak
Introduction
Prostate cancer is one of the most important cancers in men with a worldwide incidence of 25.3 per 100,000 and is the second most common cancer in men (1). The American Cancer Society (2) estimated about one in every six men will be diagnosed with prostate cancer during his lifetime. According to the society’s statistics, 238,590 new cases of prostate cancer are being diagnosed in 2013 and about 29,720 men will die of prostate cancer. In Malaysia, The Asian Pacific Prostate Society (3) reported that there were estimated 821 cases with 508 mortality cases which accounts as the second most common form of cancer among Malaysian Indian men. It is the fourth most common cause of cancer among the Chinese and Malay men.
Cancer often causes symptoms, and the treatments for cancer usually cause side effects. The diagnosis of cancer is associated with much psychological and emotional reaction like shock, anger, anxiety, confusion and depression (4). Cancer patients also have significant needs related to existing co-morbidity, uncertainty about their prognosis and the stigma associated with cancer (5).
Patients have various needs during the diagnostic, treatment, follow-up and palliative phases (6). Therefore apart from medical treatments, supportive cares are important to reduce patients’ symptoms, improve quality of life and also supporting patients and families (7). Some of the important aspects in supportive care include social care, the need for information, psychological support and spiritual needs can improve emotional and functional adjustment and symptoms and quality of life and may contribute to increased survival (8).
In order to obtain information regarding supportive care, and whether the cares are met, needs assessment is essential to determine the various supportive care needs of those patients in order to provide the best quality patient-centered care. There has been limited study on the types of supportive care needs of patients with prostate cancer, particularly in Sarawak.
The ultimate goal of this research was to conduct a needs assessment to identify the met and unmet supportive needs of patients with prostate cancer at the Urology Clinic of Sarawak General Hospital and to identify the usage of the supportive care services that are available in this hospital. It is hoped with this study, the information gathered may help the relevant authorities in future planning to address the specific priorities and unmet needs of prostate cancer patients in the management of healthcare.
Methods
The study was carried out in the Urology Clinic of Sarawak General Hospital using a cross-sectional design. This clinic is a specialist care clinic which provides consultation, treatment and follow-up care to prostate cancer patients as well as other urological conditions. Urology Clinic is chosen as the center of study because it is the biggest Urology Clinic within the state of Sarawak and is the center of referral. The clinic also refers patients for other services like welfare assistant, pain management, chemotherapy, radiotherapy, diet management etc. Within this region, there are nearly 15 to 19 new cases of prostate cancer each year. Up-to-date record shows that there are total of 132 of prostate cancer cases.
Data collection was carried out between December 2013 and February 2014. All registered patients with prostate cancer in the Urology Clinic were eligible to participate in the study. Patients who had obvious mental or intellectual impairment and physical disabilities to complete the self-report questionnaire were excluded. The researcher approached all interested patients in-person during their clinic visit, described the study to them, provided them with an information sheet and invited them to participate. The patients were asked for their willingness to complete the survey and the informed consent was obtained.
The questionnaire consists of three main components. The first component consists of question on socio-demographic data and health related profiles. The second component was the Supportive Care Needs Survey-Short Form (SCNS-SF), a revised version of Supportive Care Needs Survey (SCNS) Long Form 59. It is a 34-item self-report written questionnaire developed by Boyes (9), assesses cancer patients’ unmet needs using five domains: psychological, health system and information, physical and daily activity, patient care and support and sexuality. The need for help is rated on a 5-point scale as follows: 1= not applicable, 2= satisfied, 3= low need, 4= moderate need and 5= severe need. The SCNS is identified as one of the most comprehensive instruments for assessing the full range of needs related to health status.
The third component is the Health Service Utilization Questionnaire (HSUQ), designed to assess the type and quantity of health services used by patients. Through answering those questions, the respondents reported their use of different types of healthcare services such as social services, emergency services, specialist care, and diagnostic tests services.
Before conducting the survey, pre-testing was done using the questionnaire on patients undergoing treatment or on follow-up care for prostate cancer at the same clinic. The purpose of the pilot test was to determine the acceptability, clarity, readability and completeness of the questionnaire. Based on comments, modifications were made to improve the readability of the questionnaire.
Ethical approval was obtained from the Director of Sarawak General Hospital and Consultant Urologist. Approval also been obtained from National Research Centre (ID. 17749). The participants were informed that participation was voluntary and that they were free to discontinue participation at any time. It was stressed to the respondents that data would be handled confidentially. Informed consent was taken from each respondent.
The collected data were entered into a database. All analyses were carried out using Statistical Package for the Social Sciences (SPSS) software version 20.0. Descriptive statistics in the form of frequency counts, percentages, and mean or median scores were used to describe the patient population. Inferential statistics were used to determine the relationship between various variable. A P value of less than 0.5 (2-sided) was used to determine significant value.
Results
There was a total of one hundred thirty two registered prostate cancer patients at the Urology Clinic, Sarawak General Hospital. Out of the 132 patients, 10 patients were found out to have impaired mental health or cognitive function (n=10). There were five patients who were too sick and have to be admitted to hospital (n=5). Twenty-seven patients refused to participate in this study (n=27). Ninety-five patients completed and returned the questionnaires. The total responsive rate was 71.96%.
Table 1 provides a summary of the study participants and their socio-demographic characteristics. Out of the ninety five participants, 84.2% of them were of age 65 and above. Majority of them were married (84%). For the educational level, about 50% of them have education up to secondary level.

Full table
Based on patient perceptions of their stages of prostate cancer, 72.6% of them knew their stages of cancer. Majority of the participants have other existing health problems (84.6%).
The frequency counts for patients’ reported use of health care services documented on the HSUQ were calculated. The most frequently used healthcare services identified by the respondents were the physician specialist of 65.2%, followed by family physician or walk in clinic of 50.5%. The usage of laboratory services was 33.69% while a radiology service was 18.9%. Very few patients were referred to dietitian, physiotherapist, psychiatrist, psychologist, social worker, and public health nurse. The utilization of ambulance service was also low. None of the patient had been referred to the occupational therapist.
Table 2 shows the top ten most frequently reported unmet needs according to the SCNS-SF questionnaires. Seven out of ten unmet needs were all under the domain of health system and information. The highest unmet need (83.36%) was they wanted to know whether their cancer condition was under control or diminishing.

Full table
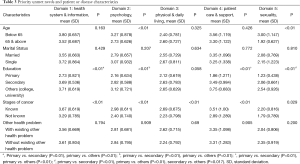
Analysis was done to determine the association between unmet needs and socio-medico characteristics of the respondents. Respondents who were older (65 years and above) had significant lower unmet needs in psychology (P<0.01), and sexuality compared to the younger group below 65 years (P<0.01). In terms of education level, except for physical and daily living, respondents with primary school level had significant lower unmet needs in all domains compared to secondary school level: health system and information (P<0.01), psychology (P<0.01), patient care and support (P<0.01), and sexuality (P<0.01). Similar results were found for respondents with known stages of cancer where higher unmet needs where found for all domains compared to their counterpart. No significant difference was found in all domains under marital status and known existing health problem (refer to Table 3).
Full table
Discussion
The top two most frequently reported unmet supportive care needs were “informed about cancer which is under control or diminishing, informed about things that can help to get well, adequately informed about the benefits and side effects of treatments” under the health system and information domain. Similar to the findings of this study, prior research also identified health and information needs as common needs among prostate cancer patients (10-12). Patients obtain source of information regarding their disease and treatments during their consultation time with the doctors. However, due to the limited time given and the conduciveness of the consultation room, many of these patients were unable to fulfil their needs. The prevalence of these three priority needs exceeded the study framework of the Supportive Care framework by Fitch (13) threshold of 30% which indicated a clinically significant unmet need that need to be addressed seriously.
“Learning to feel in control of your situation” under psychology domain was another frequently reported unmet supportive care needs of the prostate cancer patients. This finding is similar to the findings of Chambers et al. (14), Prabhu et al. (15), Bennett & Badger (16) which reported that one third of men expressed moderate to high needs for help with fears and certain degree of psychological disturbances like depression and anxiety.
More than half of the respondents reported that physician specialists and family physician were the most common healthcare service they have obtained. This is not uncommon because routine treatment and follow up would require them to meet their physicians. Nevertheless, the utilization of nutritionist, physiotherapist, psychiatrist, psychologist, social worker and public health nurses were found to be relatively low. This finding might not reflect the patients’ actual needs as these healthcare services are not commonly provided under the hospital treatment protocol, particularly in this study sample. Respondents might not aware that they can obtain these services through their healthcare providers. To get proper dietary advice from qualified health personnel is important because dietary practice can help patients to reduce bone thinning, to prevent urinary problem due to alcohol consumption, to achieve optimal health status by taking the right types of foods and supplements. Psychological support from the relevant qualified health personnel is also equally important because it will help the patients to cope with psychological and emotional stress. Occupational therapists play a critical role in helping patients of all ages to overcome the effects of disability caused by illness, ageing, post-surgery, and treatment side effect, so that patients can carry out everyday tasks or occupations without much difficulties.
The findings indicated there was no significant difference between younger and older age groups in all domains of supportive care needs except for psychology and sexuality. As expected, younger patients like any other studies before had higher needs in sexuality compared to older patients. In terms of psychology needs, older patients usually demonstrated better emotion regulation due their maturity and more inwardly focused (14,17). In this study, those who were in the age group of 65 and above probably has less work and family responsibilities as compared to their younger counterpart therefore experienced lower distress level as compared to younger age group.
Patients with higher educational level showed that they have the highest need in all domains except physical and daily living. The findings were similar to the study by Jacobs-Lawson et al. (18). Information provision for cancer patients have a positive impact on their feelings and attitudes, improved coping ability, reduction in anxiety and mood disturbances and allowing the patients to prepare for their future. Patients with a higher educational level are more likely to employ active information seeking methods like written materials and the internet to satisfy their information needs. Patients who knew their cancer stages showed higher needs in the health and information domain as compared to those who did not know their cancer stages. This could be due to the nature of the patient’s information needs may be associated with their stage in the cancer journey. Different information is needed during time of diagnosis, during treatment period and even post treatment period.
It is important to note that because the sampling was based on one regional center, this might limit the generalization of the results. Furthermore, as the data collection was based on interview, response bias is unavoidable. Nevertheless, this study provided valuable insights on the unmet needs of prostate cancer patients.
In conclusion, this study has identified unmet needs related to health and information and psychological support as the most common and important issues among the prostate cancer patients. Knowledge gained from this study may help doctors, nurses and other healthcare providers at the Urology Clinic to provide more responsive, emotionally sensitive and client-centred care for this group of patients. As this hospital is the biggest referral treatment center for prostate cancer, it is crucial that the healthcare providers acknowledge these needs in improving the delivery of health care.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Crawford ED. Epidemiology of prostate cancer. Urology 2003;62:3-12. [PubMed]
- The American Cancer Society. What are the key statistics about prostate cancer? Available online: http://www.cancer.org/cancer/prostatecancer/detailedguide/prostate-cancer-key-statistics
- Baade PD, Youlden DR, Cramb SM, et al. Epidemiology of prostate cancer in the Asia-Pacific region. Prostate Int 2013;1:47-58. [PubMed]
- Bisson JI, Chubb HL, Bennett S, et al. The prevalence and predictors of psychological distress in patients with early localized prostate cancer. BJU Int 2002;90:56-61. [PubMed]
- Prasad SM, Eggener SE, Lipsitz SR, et al. Effect of depression on diagnosis, treatment, and mortality of men with clinically localized prostate cancer. J Clin Oncol 2014;32:2471-8. [PubMed]
- Lintz K, Moynihan C, Steginga S, et al. Prostate cancer patients' support and psychological care needs: Survey from a non-surgical oncology clinic. Psychooncology 2003;12:769-83. [PubMed]
- Scotté F. The importance of supportive care in optimizing treatment outcomes of patients with advanced prostate cancer. Oncologist 2012;17 Suppl 1:23-30. [PubMed]
- Carter N, Bryant-Lukosius D, DiCenso A, et al. The supportive care needs of men with advanced prostate cancer. Oncol Nurs Forum 2011;38:189-98. [PubMed]
- Boyes A. Supportive Care Needs Survey-Short Form (SCNS-SF34). Available online: https://www.gem-beta.org/Public/MeasureDetail.aspx?mid=1592&cat=2
- Bjørnes CD, Nøhr C, Delmar C, et al. Men with prostate cancer and the accessibility to information—a literature review. OJN 2011;1:15-25.
- Davies NJ, Kinman G, Thomas RJ, et al. Information satisfaction in breast and prostate cancer patients: implications for quality of life. Psychooncology 2008;17:1048-52. [PubMed]
- Lin GA, Aaronson DS, Knight SJ, et al. Patient decision aids for prostate cancer treatment: a systematic review of the literature. CA Cancer J Clin 2009;59:379-90. [PubMed]
- Fitch MI. Supportive care framework. Can Oncol Nurs J 2008;18:6-24. [PubMed]
- Chambers SK, Newton RU, Girgis A, et al. Living with prostate cancer: randomised controlled trial of a multimodal supportive care intervention for men with prostate cancer. BMC Cancer 2011;11:317. [PubMed]
- Prabhu V, Lee T, McClintock TR, et al. Short-, Intermediate-, and Long-term Quality of Life Outcomes Following Radical Prostatectomy for Clinically Localized Prostate Cancer. Rev Urol 2013;15:161-77. [PubMed]
- Bennett G, Badger TA. Depression in men with prostate cancer. Oncol Nurs Forum 2005;32:545-56. [PubMed]
- Akechi T, Okuyama T, Uchida M, et al. Perceived needs, psychological distress and quality of life of elderly cancer patients. Jpn J Clin Oncol 2012;42:704-10. [PubMed]
- Jacobs-Lawson JM, Schumacher MM, Hughes T, et al. The relationship between lung cancer patients' educational level and evaluation of their treatment information needs. J Cancer Educ 2009;24:346-50. [PubMed]


